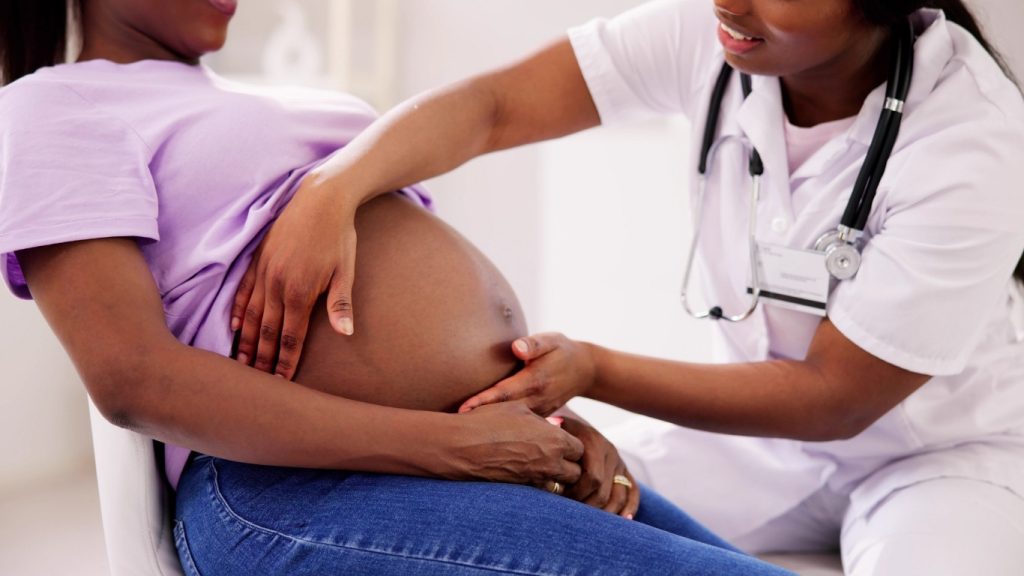
In the United States, maternal mortality remains a public health crisis with a distinctly racial dimension: Black women are far more likely to die from causes related to pregnancy and childbirth than their white counterparts, and this gap persists regardless of income or education. According to the most recent national data, non-Hispanic Black women experienced an estimated 50.3 deaths per 100,000 live births in 2023, compared with about 14.5 per 100,000 for non-Hispanic white women, CDC figures show, meaning Black mothers are more than three times as likely to die from pregnancy-related causes as white mothers.
Public health officials and researchers describe the disparity as stark and persistent. The maternal mortality rate reflects deaths that occur during pregnancy or within 42 days of the end of pregnancy from conditions caused or worsened by pregnancy. While overall U.S. maternal death rates have fluctuated in recent years, with some declines followed by modest upticks, the racial gap has changed little: Black maternal mortality remains significantly higher than that of other racial and ethnic groups.
Experts point to a range of medical, social, and systemic factors underlying this disparity. Studies indicate that chronic health conditions—such as hypertension, diabetes, and heart disease—occur at higher rates among Black women and contribute to complications during pregnancy and the postpartum period. Conditions like preeclampsia and eclampsia, serious blood pressure disorders, and postpartum cardiomyopathy, a form of heart failure, disproportionately affect Black mothers and are among the leading causes of maternal death.
Beyond individual health conditions, structural inequities in the health care system and broader society play a central role, according to public health researchers. Delayed access to high-quality prenatal care, barriers to timely care during and after delivery, and disparities in treatment within health care settings heighten the risk for Black women. Implicit bias in clinical care—the unconscious attitudes and assumptions that affect provider decision-making—has been highlighted by clinicians and patient advocates as a contributing factor.
Health officials emphasize that many pregnancy-related deaths in the United States are preventable. The Centers for Disease Control and Prevention estimates that more than 80 percent of pregnancy-related deaths could be avoided through improvements in care, early recognition of complications, and timely intervention. However, preventability does not erase the racial gap: Black women with higher levels of education and income continue to experience mortality rates well above those of white women with similar socioeconomic status. This suggests that disparities are not solely a matter of resources or individual behavior, but are also rooted in systemic inequities in care delivery and social determinants of health.
Public health organizations and policymakers have responded with efforts aimed at reducing racial disparities in maternal outcomes. Black Maternal Health Week, observed annually in April, is one initiative designed to raise awareness and promote action to improve maternal health for Black women. The CDC encourages better recognition of maternal warning signs and broader access to quality care across the prenatal and postpartum periods.
Clinicians and advocates also emphasize the importance of sustained postpartum care. Research shows that a significant portion of pregnancy-related deaths occur after childbirth, sometimes months later, underscoring the need for health care that extends beyond the traditional six-week postpartum period. Improved continuity of care during the year after delivery could help identify and treat emerging complications that contribute to maternal mortality.
Community health programs are increasingly focused on culturally competent care, patient advocacy, and reducing barriers to care in underserved areas, including maternity care deserts where obstetric services are scarce. Such efforts aim not only to provide medical services, but also to address the social and economic stresses that can increase health risks for expectant and new mothers. Public health experts argue that long-term reductions in disparities will require comprehensive strategies that integrate medical, social, and policy interventions.
For families and communities, the human toll behind the data is profound. Each maternal death represents the loss of a life, and often leaves families and children without crucial support. For Black communities, where maternal mortality rates are disproportionately high, the impact reverberates beyond individual tragedies, affecting community well-being and highlighting long-standing inequities in health and health care.
Addressing these disparities is viewed as both a medical and moral imperative by health professionals and advocates, who continue to call for sustained attention, research, and policy action to ensure that pregnancy and childbirth are safe for all women, regardless of race.