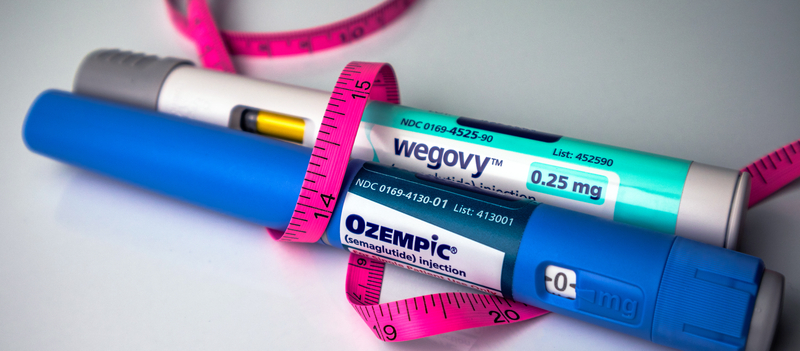
Novo Nordisk has announced plans to lower the U.S. list prices of Wegovy, Ozempic, and the oral GLP-1 medicine Rybelsus to $675 per month beginning January 1, 2027 — a notable shift for therapies that are reshaping care for obesity and type 2 diabetes. The company stated that the adjustment is intended to improve affordability for patients whose out-of-pocket costs are closely tied to list price, including individuals enrolled in high-deductible health plans and those responsible for coinsurance.
The announcement comes as GLP-1 medicines reshape care for two conditions that affect tens of millions of Americans. The CDC estimates that 40.1 million people in the United States had diagnosed or undiagnosed diabetes in 2023, and that 115.2 million adults had prediabetes. Demand for obesity treatment has also surged, even as access remains uneven, with many insurers restricting coverage and patients reporting steep out-of-pocket costs.
The planned reduction represents a significant change from current list prices, which have approached approximately $1,350 per month for Wegovy and around $1,000 for Ozempic and Rybelsus. For many patients, particularly those exposed to list price at the pharmacy counter, the adjustment may help reduce immediate financial barriers and support more consistent treatment initiation and adherence.
At the same time, affordability is shaped by more than list price alone. Coverage design, benefit structure, and utilization management policies continue to play a central role in determining real-world patient access. Research has consistently shown that patients in deductible-based or coinsurance models remain especially sensitive to list price changes, highlighting why pricing adjustments can be meaningful even when broader rebate dynamics remain unchanged.
What’s changing (and what’s not)
What’s changing, Novo Nordisk said, is that all doses of Wegovy will move to a single monthly list price of $675 in 2027, alongside Ozempic doses of 0.5 mg, 1 mg and 2 mg and Rybelsus doses of 7 mg and 14 mg. The company framed the decision as an attempt to reduce barriers for patients whose out-of-pocket costs rise and fall with the list price, particularly in benefit designs that require patients to pay the full cost until a deductible is met or to pay a percentage of the drug’s price.
What’s not changing, according to reports citing the company, is Novo Nordisk’s direct-to-patient self-pay pricing, including options that run through NovoCare Pharmacy and other access programs. Axios also reported that Novo does not expect the move to meaningfully change the net price after rebates and discounts, even if it changes what some patients pay at the counter, and said the list-price cut will not address cash prices for uninsured people in the way some readers might assume.
The distinction matters because research suggests patients can be indirectly or directly tied to list prices in common insurance designs. A JAMA Network Open study of branded drug rebates and patient out-of-pocket costs described how rising list prices paired with larger rebates can shield insurers while leaving patients, especially those facing deductibles or coinsurance, paying more based on the higher list price. That dynamic has become a flash point in the GLP-1 debate, as employers and insurers weigh whether they can afford broad coverage while patients press for more predictable access.
Federal policy is also reshaping the market ahead of 2027. A CMS fact sheet on Medicare’s drug price negotiation program lists Ozempic, Rybelsus and Wegovy with an agreed negotiated price of $274 for a 30-day supply in 2027, compared with a 2024 list price of $959 for a 30-day supply, and says about 2.282 million Medicare Part D enrollees used the drugs in 2024. Those negotiated prices apply within Medicare and do not set commercial insurance prices, but they add pressure on drugmakers and payers to justify what patients pay outside the program.
Even if the list price drops, coverage rules may remain a major gatekeeper. A January 2026 research update from the University of Pennsylvania’s Leonard Davis Institute of Health Economics warned that “coverage is more nuanced than a yes-no decision,” describing how insurers can respond to high demand and high budget impact by tightening prior authorization and other restrictions. For patients, that means a lower sticker price could arrive alongside tougher documentation requirements, narrower formularies, or step-therapy rules that still delay treatment.
Who could benefit most
These groups are most likely to see a real difference if their plan covers the medication:
-
High-deductible plan members who pay full (or near-full) price until the deductible is met
-
People with coinsurance (paying a percentage of the drug’s price rather than a flat copay)
-
Some Medicare Part D enrollees, since coinsurance designs can make out-of-pocket costs sensitive to list price
Who may not see much change
-
People with a flat copay (e.g., $25/month) may not notice a difference—because their copay is set by the plan.
-
People who are uninsured and paying cash may not benefit from this list-price change because Novo says it won’t affect direct-to-patient self-pay pricing.
-
People whose plan doesn’t cover GLP-1s for weight loss (or applies tight prior authorization rules) may still face access barriers even if list prices fall.
Health equity advocates say these coverage choices can widen disparities if access remains easiest for people with comprehensive employer plans and hardest for those in jobs with fewer benefits or those relying on Medicaid, where weight-loss coverage varies by state and is often limited. CDC data also show that obesity burdens are not evenly shared. Using combined BRFSS data from 2022 to 2024, the agency reported that 41 states, territories or D.C. had an adult obesity prevalence of 35% or higher among Black adults with sufficient data, compared with 17 among White adults and none among Asian adults, with similarly elevated prevalence in many places among Hispanic and American Indian or Alaska Native adults. These are also communities more likely to face barriers such as limited access to preventive care, higher rates of chronic disease linked to structural conditions, and insurance gaps that can make expensive medications harder to obtain.
Employer coverage patterns underscore how uneven access can be. A KFF analysis of employer survey findings reported that in 2025, one in five firms with 200 or more workers covered GLP-1 drugs for weight loss in their largest health plan, and coverage was more common among the very largest employers. For workers at smaller firms, in lower-wage jobs, or with less generous benefits, a list-price cut in 2027 may matter less than whether their plan covers the drug at all, and whether cost-sharing is structured as a flat copay or a percentage tied to the list price.
As 2027 approaches, patients, clinicians and policymakers will be watching not just the new $675 figure, but how insurers, employers and public programs decide who can realistically benefit from it.
Also Read: How Black History Month Is Being Celebrated Across the U.S.
Stay Informed. Stay Empowered.
Trending Topics
Features
- Drive Toolkit
Download and distribute powerful vaccination QI resources for your community.
- Health Champions
Sign up now to support health equity and sustainable health outcomes in your community.
- Cancer Early Detection
MCED tests use a simple blood draw to screen for many kinds of cancer at once.
- PR
FYHN is a bridge connecting health information providers to BIPOC communities in a trusted environment.
- Medicare
Discover an honest look at our Medicare system.
- Alliance for Representative Clinical Trials
ARC was launched to create a network of community clinicians to diversify and bring clinical trials to communities of color and other communities that have been underrepresented.
- Reducing Patient Risk
The single most important purpose of our healthcare system is to reduce patient risk for an acute event.
- Victor Mejia
- Jessica Wilson
- Subash Kafle